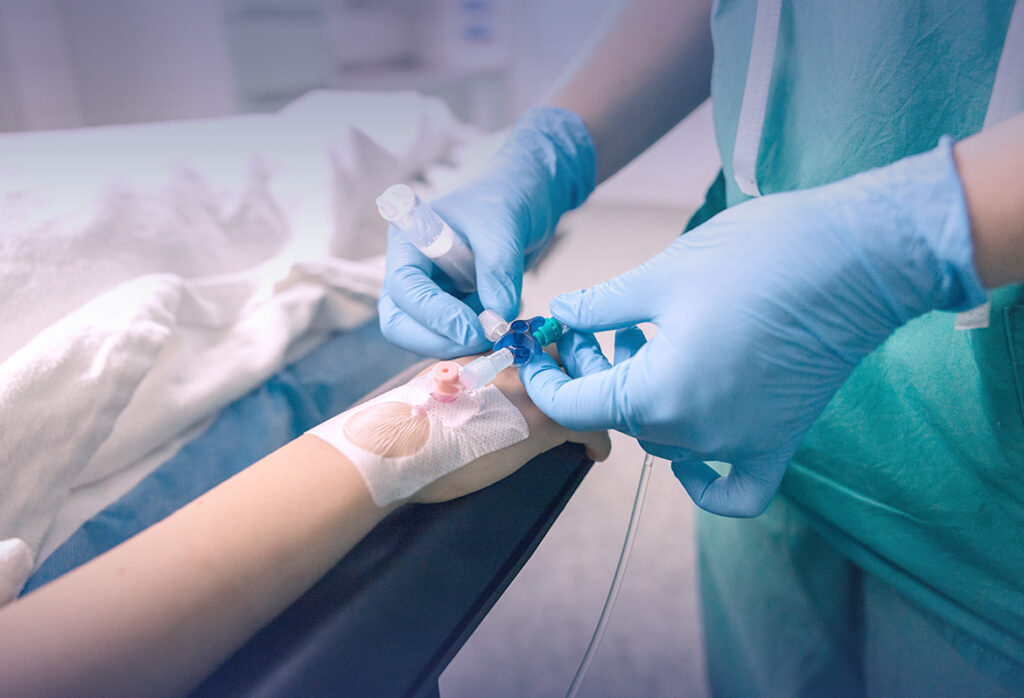
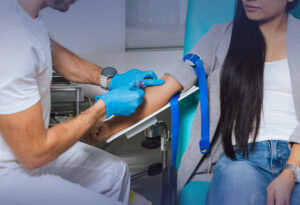
Although peripheral venous access is a common procedure, proper management requires specialized skills and adherence to specific protocols to ensure patient safety, prevent complications, and maintain catheter functionality.
How is proper management of peripheral venous access developed?
1. Choose the Insertion Site
The careful selection of the insertion site is crucial for the success of peripheral venous access. There are four key factors to consider:
- Condition of veins: The most commonly used veins are those located in the back of the hand, forearm, and wrist. It is essential to choose a vein that is palpable, straight, and of adequate caliber to accommodate the catheter
- Duration of therapy: Forearm veins are preferred for longer-term therapy, as veins in the back of the hand are more prone to complications, such as phlebitis
- Patient conditions: For patients with fragile or difficult-to-locate veins, the use of technologies, such as ultrasound, can be helpful for vein localization
- Compromised sites: Avoid veins near joints, areas with skin infections, or veins that have been used recently for other infusions. These sites can increase the risk of complications or discomfort
2. Catheter Insertion
Proper insertion of the peripheral venous catheter is essential to avoid immediate complications and ensure the durability of the line. The following steps should be followed:
- Preparation of the area: After selecting the appropriate site, the insertion area should be thoroughly disinfected using antiseptic solutions to minimize the risk of infection
- Catheter selection: The caliber of the catheter should be chosen based on the type of therapy and the condition of the vein. Smaller-caliber catheters are ideal for administering non-viscous fluids or medications, while larger catheters may be necessary for rapid infusions or the administration of thicker fluids
- Insertion technique: When inserting the catheter, it is critical to follow a strict aseptic technique and to advance the needle at an appropriate angle to minimize the risk of vein perforation and other complications
- Catheter fixation: Once the catheter is properly positioned, it should be secured using a sterile, secure transparent patch to prevent dislodgement and ensure the catheter remains in place
3. Peripheral Venous Catheter Maintenance
Regular and thorough maintenance of the peripheral venous catheter is crucial to prevent complications such as infections, occlusions, and phlebitis. The following best practices should be observed during catheter monitoring:
- Site inspection: Daily inspection of the insertion site is essential to detect any signs of infection or assess the patency of the vein. Any abnormalities should be addressed immediately to prevent worsening of the patient’s condition
- Hand hygiene: Before handling the catheter, hand hygiene is mandatory. Healthcare providers should wash their hands with an alcohol-based disinfectant or antimicrobial soap to reduce the risk of infection and prevent the transmission of communicable diseases
- Line flushing: To prevent catheter occlusion, the catheter should be flushed regularly with a sterile saline solution. The frequency and volume of flushing depend on the type of therapy, but generally, it is recommended to flush before and after medication administration to maintain catheter function
- Changing the dressing: The clear dressing covering the catheter should be replaced every 5 days or sooner if it becomes soiled, loose, or shows signs of moisture. Dressings must be replaced under sterile conditions to reduce the risk of infection
4. Prevention of Complications
Preventing complications is a critical aspect of peripheral venous access management. The most common complications include:
- Phlebitis: Inflammation of the vein, which can be prevented by selecting an appropriate insertion site, using small-caliber catheters, and limiting the duration of infusion
- Infections: These can be local or systemic. Prevention strategies include aseptic insertion techniques, proper catheter maintenance, and the use of sterile dressings
- Occlusion: Venous catheter occlusion can be prevented with regular flushing of the catheter, and, when necessary, the use of anticoagulant drugs
- Catheter dislodgement: Prevent dislodgement by securing the catheter properly with the appropriate dressings and avoiding accidental pulls or trauma to the catheter
5. Management of Complications
Despite preventive measures, complications may still arise. Timely and appropriate management is essential to minimize further issues:
- Treatment of Phlebitis: If phlebitis occurs, the catheter should be removed, and warm compresses should be applied to the affected site. In some cases, anti-inflammatory drugs or antibiotics may be necessary to manage inflammation and infection
- Infection Management: If infection is suspected, remove the catheter immediately and send it for microbiological culture. Antibiotic therapy should be initiated promptly based on the culture results and the susceptibility of the pathogen
- Occlusion Resolution: If an occlusion occurs, thrombolytic agents may be required, or the catheter might need to be replaced. It is crucial never to force infusion through an obstructed catheter, as doing so can lead to catheter rupture or the migration of emboli
- Management of Dislodgement: If the catheter becomes dislodged, it should be removed and, if necessary, reinserted at a new site. To prevent further dislodgement, it is important to provide proper education to both patients and healthcare personnel about catheter handling
6. Removal of the Peripheral Venous Catheter
Catheter removal is a simple procedure, but it must be performed carefully to avoid complications.
Directions for Removal
The catheter should be removed when it is no longer needed, when the insertion site shows signs of infection or inflammation, or if the catheter is obstructed or dislodged.
Removal Procedure
The catheter should be removed under aseptic conditions. After removal, the site should be compressed for several minutes to prevent bleeding, and then covered with a sterile dressing.
Post-Removal Monitoring
Following removal, the insertion site must be monitored for signs of infection or hematoma. It’s also crucial to educate the patient to report any suspicious symptoms promptly. The patient should be aware of signs of complications and know when to contact healthcare professionals.
7. Patient Education
Patient education is essential in the management of peripheral venous access. Patients should be well-informed about the following key points:
- Signs of Complications: It is essential for patients to recognize signs of infection, phlebitis, or occlusion and understand when to contact healthcare professionals for further evaluation
- Care of the Insertion Site: Patients should be educated on how to maintain a clean and dry insertion site, avoid actions that could cause the catheter to become dislodged, and be able to identify any potential issues early
- Importance of Hygiene: Patients must comprehend the significance of proper hand hygiene and site cleanliness to prevent infections and maintain catheter integrity
Peripheral venous access management is a crucial aspect of healthcare, demanding specialized skills and ongoing attention to ensure both patient safety and catheter functionality.
By adhering to established guidelines and best practices, healthcare providers can significantly minimize the risk of complications and enhance patient outcomes. Proactive and meticulous management, coupled with thorough patient education, plays a pivotal role in the success of treatment and patient comfort, ultimately contributing to a safer and less stressful hospital experience.